Reasons to Have a Podiatrist on Your Medical Care Team
The reason a podiatrist should be on your medical care team is you use your legs and feet a lot. Seriously, the average person walks around 1,200 miles and climbs about 27,400 stairs a year–a lot can go wrong. Overuse, ill-fitting shoes, injuries, and chronic medical conditions–like arthritis or diabetes–can all lead to pain that requires a foot specialist.
If you are experiencing foot and ankle pain, it might be time to see a podiatrist. Do you go to your general practitioner for physical therapy? Each body part has a specialized doctor, and so do the feet. The unique doctor in charge of this critical area is a podiatrist. You might need to see a podiatrist and not even know it.
In this article, we will discuss what a podiatrist does, what podiatric medicine is, and the benefits of seeing a podiatrist. There are many reasons why a podiatrist should be a part of your medical care team. We provide truly comprehensive foot and ankle care at Foot & Ankle Specialists of Illinois.
 What Does a Podiatrist Do?
What Does a Podiatrist Do?
Podiatrists do many of the same things as you and me. They eat, drink water, sleep, and love, but they also save millions of people from a lifetime of pain, frustration, and sometimes even death. A podiatrist should be a part of your medical care team because they specialize in preventing, diagnosing, and treating foot and lower-leg disorders—podiatric medicine addresses conditions caused by injury and ongoing health issues like diabetes. You might know them as your podiatric physician or doctor of podiatric medicine. Either way, they treat patients of all ages.
What does a podiatrist do during an assessment? When you go to your first appointment, your podiatrist will probably watch how you stand and walk to check several things, including your range of motion among other things. They do this to get a sense of your mobility and any pressing concerns they can readily see. The benefits of seeing a podiatrist are numerous, and include prevention, diagnosis, and treatment of:
- Fractures
- Sprains
- Bunions
- Hammertoes
- Nail disorders
- Growing pains
- Heel pain
- Morton’s neuroma
- Foot deformities
- And complications related to diabetes and arthritis
In case you didn’t know, Morton’s neuroma is the thickening of tissues around a nerve leading to your toes, and it can feel excruciating. You might have Morton’s neuroma if you are experiencing pain, swelling, a burning feeling, cramped toes, and potentially even difficulty walking.
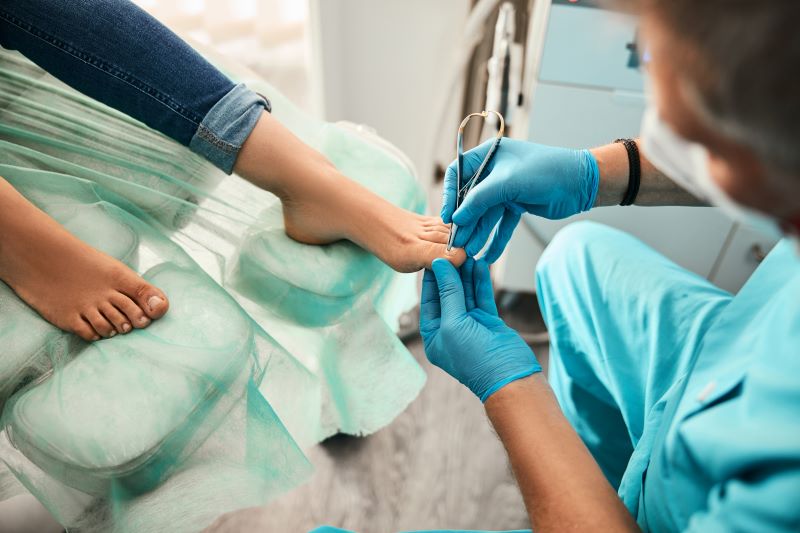 Podiatric Medicine
Podiatric Medicine
Podiatric medicine is a growing medical-sciences branch devoted to preventing, diagnosing, and treating foot disorders commonly resulting from injury or disease. It seems like common sense that preventive healthcare applies to your entire body, but it’s hard to imagine how important a role your feet play. Believe it or not, your foot and the rest of your body share a complex, vital interrelation. Because of this, your podiatrist may spot potential health issues first, as your feet are often the first to show signs of severe conditions. Your podiatrist should be passionate about helping you understand how your lifestyle affects your foot health and recommend helpful changes regardless of age or activity level.
A student studying to be a Doctor of Podiatric Medicine (D.P.M.) attends an accredited college of podiatric medicine. This 4-year degree includes classroom instruction and laboratory work. Then, they complete clinical science courses and gain practical experience within community clinics and accredited hospitals. After D.P.M. school, students attend a 36-month residency to gain competency-based medical and surgical experiences in rearfoot and ankle surgery.
At a minimum, your Doctor of Podiatric Medicine will perform a gait analysis, conduct tests, and recommend treatments, orthotics, or changes to your footwear. Their focus is supporting the long-term health and strength of your feet. Podiatrists will often specialize in a particular area of podiatric medicine: senior care, pediatrics, orthopedics, surgery, sports, biomechanics, etc. Diabetic care, for example, is a growing and vital specialization due to the connection between diabetes and several severe problems occurring in the lower limbs.
Signs You Need Podiatric Medicine:
- Pain, numbness, or swelling in your feet
- Nail fungus
- Constant heel pain
- Athlete’s foot that won’t go away
- A broken or sprained ankle or foot
- Diabetes
- Joint pain in the foot or ankle
- A sports injury
 Benefits of Seeing a Podiatrist
Benefits of Seeing a Podiatrist
The benefits of seeing a podiatrist go far beyond preventing, diagnosing, and treating foot and lower-leg disorders like sprains, nail disorders, and growing pains. A critically important reason why a podiatrist should be a part of your medical care team is that foot problems are often an indication of other potentially much more severe conditions. Diabetes, for instance, damages nerves and reduces blood flow to your feet and legs. Across the globe, a limb amputation occurs every 30 seconds, and a staggering 85% of these amputations are primarily associated with two diabetic conditions: diabetic neuropathy and peripheral artery disease (PAD).
As discussed above, Doctors of Podiatric Medicine are often the first to notice symptoms of a severe disorder, so it’s important to consider why a podiatrist should be a part of your medical care team.
Benefits Include:
- Reduced nerve problems
- Relief from pain and infections
- Help identifying possible health conditions
- Support for long-term foot health
- Promotion of healthy, long-lasting lifestyle changes
Relief from heel pain is a specific top benefit of seeing a podiatrist. Heel spurs are a common cause of even more common heel pain. A buildup of calcium at the bottom of your heel bone and heel spurs can have several causes: running, ill-fitting shoes, or being overweight. Plantar fasciitis, another common cause of heel pain, is inflammation in the connective tissue running along the bottom of your foot. Nonsupportive shoes wreak havoc on your feet and lead to overpronation and numerous other conditions. So, what does a podiatrist do to treat it? Commonly, treatment starts with over-the-counter pain medications and shoe inserts, aka orthotics. In the most extreme cases, your podiatrist might suggest surgery.

